- Home
- About Us
- Housing
- Resources
- Contact Us
-
-
-
Address: 223 S. Winnebago Street Rockford, IL 61102
Phone: 815-489-8500
-
-
- Updates
-

Address: 223 S. Winnebago Street Rockford, IL 61102
Phone: 815-489-8500
Address: 223 S. Winnebago Street Rockford, IL 61102
Phone: 815-489-8500









Viruses constantly change through mutation, and new variants of a virus are expected to occur over time. Sometimes new variants emerge and disappear. Other times, new variants emerge and persist. Multiple variants of the virus that causes COVID-19 have been documented in the United States and globally during this pandemic.
The virus that causes COVID-19 is a type of coronavirus, a large family of viruses. Coronaviruses are named for the crown-like spikes on their surfaces. Scientists monitor changes in the virus, including changes to the spikes on the surface of the virus. These studies, including genetic analyses of the virus, are helping scientists understand how changes to the virus might affect how it spreads and what happens to people who are infected with it.
The B.1.617.2 and B.1.1.529 variants circulating in the United States are classified as variants of concern.
These variants seem to spread more easily and quickly than other variants, which may lead to more cases of COVID-19. An increase in the number of cases will put more strain on health care resources, lead to more hospitalizations, and potentially more deaths.
So far, studies suggest that antibodies generated through vaccination with currently authorized vaccines recognize these variants. This is being closely investigated and more studies are underway.
Rigorous and increased compliance with public health mitigation strategies, such as vaccination, physical distancing, use of masks, hand hygiene, and isolation and quarantine, is essential to limit the spread of the virus that causes COVID-19 and protect public health.
For more information please visit: https://dph.illinois.gov/covid19/data/variants
“We should anticipate that we very well may get another variant that would emerge, that would elude the immune response that we’ve gotten from infection and/or from vaccination,” Fauci said at an event with the USC Annenberg Center for Health Journalism this week.
Dr. Anthony Fauci warned Americans to “not be surprised” if a new, more dangerous COVID-19 variant emerges this winter. Looking at numbers, the hospitalization and deaths are currently down nationwide at a seven-day moving average in the US of 323. Comparing it to February and March of this year when the U.S was at 1,00 to 2,500 according to data from the Centers for Disease Control and Prevention.
Fauci explained to Americans that they shouldn’t have their guard down just yet because of the winter season and its wave of illness. “It looks like we’re going in the right direction,” he said, adding: “However, I think it would be a bit cavalier to all of a sudden say, ‘We’re completely through with [the pandemic].’”
“We’re encouraging people, particularly as we’re now in the fall season, to get that particular updated vaccine, which fortunately for us is directed at the major circulating variant,” Fauci said.
Hospitals across the nation are bracing themselves for the season of viruses. According to the CDC the yearly Flu Cases are already rising in parts of the U.S. and while COVID-19 is still impacting the world. “If you go around the nation and ask hospitals how busy they are, every single one of them will tell you: They’re busy,” said Dr. Carlos del Rio, an executive associate dean at the Emory University School of Medicine and Grady Health System in Atlanta.
Despite the shortages in the healthcare system like capacity, staffing, and supplies, hospital leaders are saying morale is “actually pretty good,” McDeavitt said. “We’ve moved on from early in the pandemic, wondering if we were going to get sick and potentially die.”
“I think those worries are alleviated,” McDeavitt said. “We know how to handle it now.”
During the winter season, The CDC recommends an annual flu shot for everyone aged 6 months and older. Children younger than age 9 who have never had a flu vaccine, the CDC said, should get two this year, at least four weeks apart and of course getting the COVID-19 vaccine and booster shots.
Given the nation’s diminished immunity and current BA.5 surge, more people are wondering whether they should get a booster (or second booster) now, or if they should wait until the fall when a new shot will likely be available. Here’s what to know.
“If you get a booster now, it does reduce your risk of getting infected [with BA.5],” said Dr. Ashish Jha, the White House COVID-19 response coordinator, during the briefing. “It does not drive it to zero, but it reduces that risk. And the data are very clear that if you are over 50, that extra booster dramatically lowers the risk of getting into the hospital, going to the ICU, or dying. There are very few things we do in medicine that have the kind of benefit we see from that extra shot.”
Who should get a booster?
Currently, the U.S. Food and Drug Administration (FDA) and U.S. Centers for Disease Control and Prevention (CDC) recommend one booster shot for everyone ages 5 and older who are five months out from their last COVID-19 vaccine dose, and second booster doses for people ages 50 and older at least four months after their first booster. (Additional boosters are recommended for people with weakened immune systems).
Should people wait for the Omicron booster in the fall?
On June 30, the FDA decided that the next COVID-19 booster needs to target the Omicron subvariants BA.4 and BA.5 specifically, because such a booster would likely increase people’s protection from getting infected with Omicron, and hopefully extend that protection to longer than a few months.
“The threat to you [from BA.5] is now,” said Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases and the White House’s chief COVID-19 medical officer, in a briefing on July 12. “If you are not vaccinated to the fullest—namely, not gotten boosters according to the recommendations—you are putting yourself at increased risk.”
Getting boosted now “does not preclude you from also getting an [Omicron-specific] booster in the fall,” he added. “If the risk is now, address the current risk.”
You can read the full article here:
To be clear, all health officials are in universal agreement — the potential list of symptoms for those affected by an Omicron SARS-CoV-2 infection remains largely the same. Janice Johnston, M.D., co-founder and chief medical officer at Redirect Health, says that the Omicron variant may infect individuals differently, but that it’s not uncommon for subsequent symptoms to be the same as those we’ve seen earlier in the pandemic. “We’ve seen this for years with the influenza virus; every patient is not the same in terms of holistic health, immunity level and ability to fight the virus,” she adds.
While the list of potential symptoms related to Omicron infections is the same, limited data suggests that a few symptoms — chiefly fatigue, feeling overtired or exhausted and pain across multiple muscle groups on the body — are much more common than breathlessness or a loss of taste and smell associated with previous strains of the coronavirus.
But most of the research being presented currently is limited and comes from anecdotes from healthcare providers on the ground in South Africa, explains Nicholas Kman, M.D., an emergency medicine physician at the Ohio State University Wexner Medical Center.
As we approach Summer, COVID-19 remains a part of our lives. As we shift from a pandemic to an endemic state, we will need to retool to allow us to live with the reality of the virus. As we look to Summer 2022, we are in a much different position than in Spring 2020. Vaccines, boosters, and new viral treatments provide us with tools not at our disposal two years ago. In addition, vigilance with masks remains an integral part of our country’s response. RHA continued to require mask requirements indoors for all staff, community members, and visitors, regardless of vaccination status. I believe it has served our residents and us well.
As the trajectory of the COVID-19 pandemic continues to unfold, government officials at all levels are reevaluating health and safety protocols and adjusting workplace guidance based on the ever-shifting case and vaccination metrics. Therefore, beginning Tuesday, May 31st, 2022, RHA will return to “Business as usual” except for our development community rooms and temperature readings. We will open our office doors to regular business hours. We will resume in-person meetings without occupancy restrictions and lift mask mandates.
Our development community rooms and computer labs will now open at 8:00 am without the restriction of occupancy. However, we will close each room daily at 4:00 pm to allow our maintenance staff to sanitize the space. In doing so, each site will need to ensure that our sanitizing stations remain fully stocked, and we encourage our residents to use the supplies to sanitize areas after use.
RHA offices will be open to the public without the requirement of an appointment, and we will resume regular business hours. All safeguards will remain in place in meeting areas. Because temperatures are not noticeable, we will continue requiring temperature readings when entering our facilities and ask those with a fever not to enter the RHA offices.
As we always have, we encourage you to protect yourself, get vaccinated, and continue wearing your mask. However, most importantly, please stay home if you are not feeling well.
As we have done throughout, we will continue to communicate with the community through periodic messages with updated information as it becomes available. Please also look to RHA’s COVID-19 page for the most current information.
Stay safe, Thank you,
Laura Snyder
Chief Executive Officer
November 19th Dr. Rochelle Walensky, director of the CDC, supported an advisory committee’s advice and expanded the group of people who can now get a COVID-19 Booster shot to include all adults over 18.
Since more people are now eligible to get the booster dose, people question if they need one immediately or if the initial vaccination is no longer working. The CDC states that “all adults who had received the Pfizer-BioNTech or Moderna vaccine are eligible to get a booster at least six months after their second dose.” However, before the CDC made a clear distinction between those over the age of 65 and with underlying health conditions, they said they “should” get a booster shot and those living in high-risk areas who “may” get the booster shot.
Dr. Anthony Fauci tells TIME that “I came down very strongly that I thought saying ‘should’ vs. ‘may’ has done nothing but confuse people,” he says. “If you want people to get a booster, just tell them what to do.”
“Right now, we are facing more than 90,000 new infections a day [on average], we are entering the winter season, and people are gathering for the holidays,” says Dr. Leana Wen, professor of health policy and management at George Washington University. “We know immunity to symptomatic infection wanes substantially at the six-month mark, and immunity even to severe disease wanes too. It’s mind-blowing to me that we cannot just be straightforward with people at this point and say it is essential to get a booster. The CDC playing around with ‘should’ vs. ‘may’ wording has further confused people.”
The urgency to get a booster shot isn’t as great as the urgency to get fully vaccinated. Studies show that the initial doses of all three vaccines continue to protect people from needing to be hospitalized. The agency’s decision to recommend booster shots is because of growing evidence from countries like Israel that infections among vaccinated people are possible and that some people are sick enough to go to the hospital.
The bottom line, getting the booster shot is your choice. It is something that could affect friends and family and be an added layer of protection for yourself. The stigma that the booster shot is somewhat of a luxury and not something people need to get “needs to change urgently,” states Wen.

OCTOBER 26, 2021
U.S. Department of Health and Human Services
If you have a compromised immune system, CDC recommends you get a third dose of mRNA COVID-19 vaccines at least 28 days after your second dose.
Learn About Booster Shots
When searching for a vaccine provider, there is no difference between looking for your first shot or any other doses. That means if you’re eligible, you can get your booster shot anywhere that provides COVID-19 vaccines approved for boosters.
What You Need to Know
COVID-19 Vaccine booster shots are available for the following Pfizer-BioNTech vaccine recipients who completed their initial series at least 6 months ago and are:
Data Supporting Need for a Booster Shot
Studies show that after getting vaccinated against COVID-19, protection against the virus may decrease over time and be less able to protect against the Delta variant. Although COVID-19 vaccination for adults aged 65 years and older remains effective in preventing severe disease, recent data pdf icon[4.7 MB, 88 pages] suggest vaccination is less effective at preventing infection or milder illness with symptoms. Emerging evidence also shows that among healthcare and other frontline workers, vaccine effectiveness against COVID-19 infections is decreasing over time. This lower effectiveness is likely due to the combination of decreasing protection as time passes since getting vaccinated (e.g., waning immunity) as well as the greater infectiousness of the Delta variant.
Data from a small clinical trial show that a Pfizer-BioNTech booster shot increased the immune response in trial participants who finished their primary series 6 months earlier. With an increased immune response, people should have improved protection against COVID-19, including the Delta variant.

ADOLESCENTS AGES 12–18
A new MMWR report finds that for adolescents ages 12–18, two doses of Pfizer-BioNTech Vaccine are 93% effective at preventing COVID-19 hospitalization. These findings show how important vaccination is to protect U.S. adolescents against severe COVID-19. Learn more: bit.ly/MMWR7042e1.
Among hospitalized U.S. patients aged 12–18 years, vaccine effectiveness of 2 doses of Pfizer-BioNTech vaccine against COVID-19 hospitalization during June–September 2021, was 93% (95% confidence interval = 83%–97%).
What are the implications for public health practice?
This evaluation demonstrated that 2 doses of Pfizer-BioNTech vaccine were highly effective in preventing COVID-19 hospitalization among persons aged 12–18 years. Findings reinforce the importance of vaccination to protect U.S. youths against severe COVID-19.
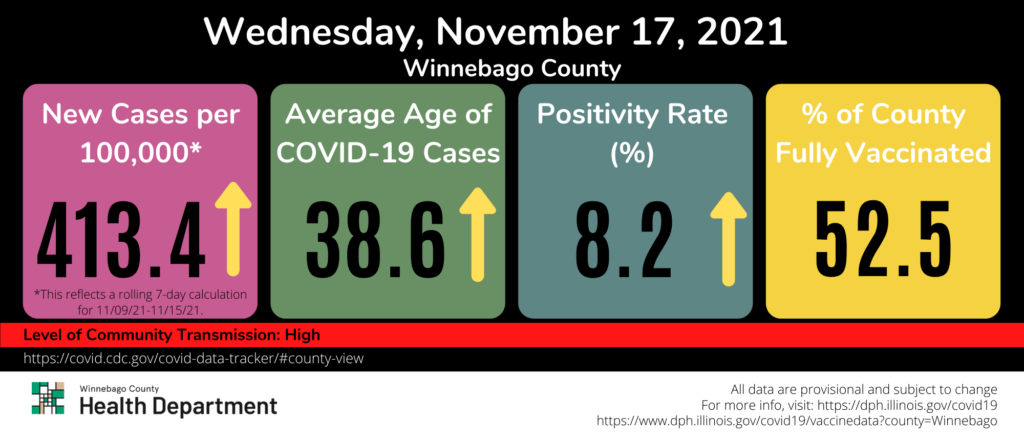
Winnebago County is now at HIGH Community level.
Wear A Mask while in public indoor settings, regardless of your vaccination status
Avoid Crowded Indoor Settings.
 your vaccinations: it is important to get your COVID-19 vaccination and your eligible booster shots
your vaccinations: it is important to get your COVID-19 vaccination and your eligible booster shotsThe Community Level is high because the levels of COVID-19 hospitalizations, cases, and patients in hospital beds are a strain for the local health system. Learn more about COVID-19 Community Levels

Governor JB Pritzker officially reinstated an indoor mask mandate, regardless of vaccination status, today during a news conference in Chicago. The mandate will start Monday, August 30th 2021. Please view this link to see the full conference: https://illinoisnewsroom.org/press-briefing-on-covid-19/
While the State of Illinois Phase 5 is set to mark a full reopening beginning on June 11, not all restrictions will be lifted. The State will lift its outdoor mask requirement for schools in line with the U.S. Centers for Disease Control and Prevention guidance. Fully vaccinated people should continue to get tested if experiencing COVID-19 symptoms.
The State has also advised that businesses and other venues should continue to allow for social distancing to the extent possible, especially indoors. Businesses and venues may also continue to put in place additional public health mitigations as they deem appropriate, including requiring face coverings. This means wearing masks or physically distancing, where federal, state, local, tribal, or territorial laws, rules, and regulations are required, including local business and workplace guidance. “While the updated guidance from the CDC is welcome news, let me remind everyone that this guidance is only for those people who are fully vaccinated,” said IDPH Director Dr. Ngozi Ezike. “Individuals who do not have the protection afforded by one of the safe and effective COVID-19 vaccines should still wear a mask.”
To protect the health and continued welfare of the Rockford Housing Authority’s employees, residents, and guests, RHA will continue Covid 19 protocols for social distancing and mask mandates on all RHA Properties. Many of our residents are elderly and still at risk. Covid 19 best practices will be applied in common areas such as reception areas, community rooms, conference rooms, restrooms, and line/queuing until further notice.
While removing occupancy limits and other rules represents a step forward in the COVID pandemic, state officials have continued to caution all residents that it is possible for the State to move back to previous phases.
A properly fitted mask can provide some added protection over a poorly fitting mask for both the wearer and other people. The primary intent of mask use is to suppress the spread of virus from the wearer to other people. Because COVID-19 can be spread by people who display characteristic symptoms and by those who do not exhibit any symptoms, broad mask use is encouraged to minimize the spread from those who are sick (or potentially sick) to others.
The mask, if worn properly and consistently, also helps protect healthy people from catching the disease when they are in close proximity to people who are sick. It may also provide protection to the wearer from aerosols that persist in poorly ventilated environments, such as an elevator.
Information about how long virus-carrying droplets can persist in the air is being updated regularly. Some research suggests that droplets can remain airborne for multiple hours. So do your part to protect yourself and others by wearing well-fitting, protective masks.
The simple answer is NO. Wearing a mask, in part, is meant to protect your respiratory system (your lungs, throat, and sinuses) from direct exposure to airborne droplets and particles that may contain the virus.
To do this, one must protect the primary entry points to your lungs and throat—your nose and mouth. Therefore, leaving your nose exposed will provide an easy pathway for airborne particles to enter your system (by inhaling through your nose) or for droplets to exit your system (by exhaling, sneezing, etc.), potentially endangering those around you.
Absolutely. Even with a mask, you should still make every effort to stay at least 6 feet away from people who don’t live with you. Masking is only one layer of protection, and it’s an imperfect one. Social distancing isn’t foolproof, either, but the more layers of protection you can employ, the safer you’ll make yourself and everyone else around you.
Illinois News
Gov. Pritzker Aligns Illinois Mask Guidance with CDC for Fully Vaccinated People
Administration to Rescind Emergency Public Health Rules Following New CDC Guidance; CDC: Fully Vaccinated People No Longer Need to Wear a Mask in Most Instances or Practice Social Distancing
Monday, May 17, 2021 – the Governor of the State of Illinois.
SPRINGFIELD – Following guidance from the CDC that fully vaccinated people can stop wearing a mask and practicing social distancing in most indoor and outdoor settings, Governor JB Pritzker and the Illinois Department of Public Health have announced that Illinois will align state executive orders with the latest CDC guidance and rescind IDPH emergency rules enforcing masking and distance.
The CDC continues to require masks for everyone in healthcare settings, in congregate settings and on transit. In addition, in line with CDC guidance, the Illinois State Board of Education and Illinois Department of Public Health require masks in schools. The Illinois Department of Children and Family Services requires masks in daycare.
“Getting vaccinated is the ultimate protection from COVID-19 and the quickest ticket back to normal life,” said Governor JB Pritzker. “With public health experts now saying fully vaccinated people can safely remove their masks in most settings, I’m pleased to follow the science and align Illinois’ policies with the CDC’s guidance. I also support the choice of individuals and businesses to continue to mask out of an abundance of caution as this pandemic isn’t over yet.”
“While the updated guidance from the CDC is welcome news, let me remind everyone that this guidance is only for those people who are fully vaccinated,” said IDPH Director Dr. Ngozi Ezike. “Individuals who do not have the protection afforded by one of the safe and effective COVID-19 vaccines should still wear a mask. While more than 64% of adults in Illinois have received at least one dose of a COVID-19 vaccine, we need to increase that number. To slow down disease spread and the development of even more deadly variants, we need as many people as possible to be vaccinated.”
The Governor is issuing an updated executive order to remove the mask requirement for fully vaccinated people in most settings, and the Illinois Department of Public Health is rescinding emergency rules in the Control of Communicable Disease Code that enforce masking and distancing for vaccinated people in business settings. In line with CDC guidance, individuals who are unvaccinated should continue wearing masks in most settings and both vaccinated and unvaccinated individuals should continue to wear masks on public transportation, in congregate facilities, and in healthcare settings.
As of today, more than 4.8 million Illinoisans are fully vaccinated, and 58% of residents 16+, 64% of residents 18+ and 86% of residents 65+ have received their first dose.
LATEST CDC GUIDANCE
The CDC still recommends that unvaccinated people continue to take preventive measures, such as wearing a mask and practicing social distancing. In their latest guidance, the CDC now reports that indoor and outdoor activities pose minimal risk to fully vaccinated people and that fully vaccinated people have a reduced risk of transmitting SARS-CoV-2 to unvaccinated people.
Fully vaccinated people can:
For now, fully vaccinated people should continue to:
“If an individual is experiencing symptoms of COVID-19 including fever, shortness of breath and cough, they call their healthcare provider.
The healthcare provider will consider these symptoms, travel history, possible exposure to a known case, and any underlying health conditions specific to that patient when evaluating the need for testing for COVID-19. If COVID-19 testing is needed, healthcare providers collect the specimens that are then sent to a State or private lab for testing.
The healthcare provider will determine if you need to be tested for COVID-19 and may recommend that you stay home and provide self-care if you have mild symptoms. Those individuals who have no symptoms, do not need to be tested.
The positive cases of COVID-19 reported by the Illinois Department of Public Health and the Winnebago County Health Department include all positive tests that were submitted to the state or private lab for testing.”

Venues and meeting spaces can resume. Multiple groups are permitted given facilities have space to appropriately social distance and can limit interaction between groups. This includes activities such as conferences and weddings
Revised guidelines to allow select indoor recreation facilities (e.g., bowling alleys, skating rinks), as well as clubhouses to reopen. Concessions permitted with restrictions.
Indoor dining can reopen with groups of 10 or less, with tables spaced 6-feet apart in seated areas and with standing areas at no more than 25% of capacity.
Can reopen with no more than 25% occupancy, and with interactive exhibits and rides closed; guided tours should be limited to 50 people or fewer per group; museums should have a plan to limit congregation via advance ticket sales and timed ticketing; concessions permitted with restrictions.
Can reopen with no more than 25% occupancy, and with interactive exhibits, indoor exhibits, and rides closed; guided tours should be limited to 50 people or fewer per group; zoos should have a plan to limit congregation via advance ticket sales and timed ticketing; concessions permitted with restrictions.
Indoor seated theaters, cinemas, and performing arts centers to allow admission of the lesser of up to 50 guests OR 50% of overall theater or performance space capacity (applies to each screening room); outdoor capacity limited to 20% of overall theater or performance space capacity; concessions permitted with restrictions.
Outdoor spectator sports can resume with no more than 20% of seating capacity; concessions permitted with restrictions.
Allow no more than 50% of sound stage or filming location capacity; crowd scenes should be limited to 50 people or fewer.
Revised guidelines allow competitive gameplay and tournaments; youth and recreational sports venues can operate at 50% of facility capacity, 20% seating capacity for spectators, and group sizes up to 50 with multiple groups permitted during practice and competitive games given venues have space to appropriately social distance and can limit interaction between groups; concessions permitted with restrictions.
Revised guidelines allow gyms to open at 50% capacity and allow group fitness classes of up to 50 people with new safety guidelines for indoors, with multiple groups permitted given facilities have space to appropriately social distance and can limit interaction between groups.
Water-based activities permitted in accordance with IDPH guidelines; no more than 50% of facility capacity with group size of no more than 15 participants in a group, unless participants changing weekly.
For more resources please visit the Illinois Department of Public Health COVID-19 Page here: https://www.dph.illinois.gov/covid19
Coronavirus disease 2019 (COVID-19) is a a respiratory illness that can cause mild to severe illness in people. The Winnebago County Health Department, along with our local healthcare partners, local health departments in the region, the Illinois Department of Public Health (IDPH) and the Centers for Disease Control and Prevention (CDC) are working to contain the spread of COVID-19 and protect the public’s health.
For the latest information please visit: https://www.wchd.org/covid-19#:~:text=Recent%20Updates%20on%20COVID%2D19,Click%20here%20for%20guidance
ACIP and CDC are making recommendations for who should be offered COVID-19 vaccine first when supplies are limited. While CDC makes recommendations for who should be offered COVID-19 vaccine first, each state has its own plan for vaccine prioritization, distribution, and allocation.
Please contact your state health department for more information on its plan for COVID-19 vaccination.
For COVID-19 Vaccination Updates visit: https://www.cdc.gov/coronavirus/2019-ncov/vaccines/faq.html
For more FAQs visit this link: https://getvaccineanswers.org/
Both this disease and the vaccine are new. We do not know how long protection lasts for those who get infected or those who are vaccinated. Experts are working to learn more about both natural immunity and vaccine-induced immunity. CDC will keep the public informed as new evidence becomes available.
· The potential serious risk COVID-19 infection poses to them and their loved ones if they get the illness or spread it to others. Remind them of the potential for long-term health issues after recovery from COVID-19 disease.
· Scientists are still learning more about the virus that causes COVID-19. And it is not known whether getting COVID-19 disease will protect everyone against getting it again, or, if it does, how long that protection might last.
· The vaccine was tested in large clinical trials and what is currently known about its safety and effectiveness.
· The vaccine is not a perfect fix. You will still need to practice other precautions like wearing a mask, social distancing, handwashing, and other hygiene measures until public health officials say otherwise.
COVID-19 vaccines were tested in large clinical trials to make sure they meet safety standards. Many people were recruited to participate in these trials to see how the vaccines offers protection to people of different ages, races, and ethnicities, as well as those with different medical conditions.
· The Food and Drug Administration (FDA) carefully reviews all safety data from clinical trials and an authorizes emergency vaccine use only when the expected benefits outweigh potential risks.
· The Advisory Committee on Immunization Practices (ACIP) reviews all safety data before recommending any COVID-19 vaccine for use.
· FDA and CDC will continue to monitor the safety of COVID-19 vaccines, to make sure even very rare side effects are identified.
According to the CDC, the COVID-19 vaccine will be given to U.S. citizens at no cost, Yacoub confirms. Some vaccine providers may decide to charge an additional fee for administering the shot, but this fee can be reimbursed by recipients’ insurance, or, if uninsured, the Health Resources and Services Administration’s Provider Relief Fund
Most people do not have serious problems after being vaccinated. We will understand more about mild side effects of the COVID-19 vaccine before we start to use it. However, your arm may be sore, red, or warm to the touch. These symptoms usually go away on their own within a week. Some people report getting a headache or fever when getting a vaccine. These side effects are a sign that your immune system is doing exactly what it is supposed to do. It is working and building up protection to disease.
· A fever is a potential side effect and when they should seek medical care.
· Symptoms typically go away on their own within a week. Also let them know when they should seek medical care if their symptoms don’t go away.
· The vaccine cannot give someone COVID-19.
· The side effects are a sign that the immune system is working.
COVID-19 vaccines are being tested in large clinical trials to assess their safety. However, it does take time, and more people getting vaccinated before we learn about very rare or long-term side effects. That is why safety monitoring will continue. CDC has an independent group of experts that reviews all the safety data as it comes in and provides regular safety updates. If a safety issue is detected, immediate action will take place to determine if the issue is related to the COVID-19 vaccine and determine the best course of action.
· The FDA and CDC are continuing to monitor safety, to make sure even long-term side effects are identified.
· COVID-19 vaccines will be continuously monitored for safety after authorization, and ACIP will take action to address any safety problems detected.
All but one of the COVID-19 vaccines currently in phase 3 clinical trials use two shots. The same vaccine brand must be used for both shots.
· Nearly all COVID-19 vaccines being studied in the United States require two shots. The first shot starts building protection, but everyone has to come back a few weeks later for the second one to get the most protection the vaccine can offer.
· Two shots are generally needed to provide the best protection against COVID-19 and that the shots are given several weeks apart. The first shot primes the immune system, helping it recognize the virus, and the second shot strengthens the immune response.
The two COVID-19 vaccines currently available in the United States do not contain eggs, preservatives, or latex.
For a full list of ingredients, please see each vaccine’s,
Fact Sheet for Recipients & Caregivers:
· Pfizer-BioNTech COVID-19 vaccineexternal
· Moderna COVID-19 vaccineexternal
Notable Differences:
· Age minimum: The vaccine developed by Pfizer and BioNTech is approved for people age 16 and older, and the vaccine developed by Moderna is approved for people age 18 and older
· Storage requirements: Moderna does not require ultra-cold storage [like Pfizer doses do], making it easier to store while the Moderna vaccine can be stored in a freezer or refrigerator, the Pfizer vaccine needs to be stored in a special container in very cold temperatures. This discrepancy won’t affect you directly but is more the concern of healthcare facilities.
Serious problems from vaccination can happen, but they are rare. CDC has learned of reports that some people have experienced severe allergic reactions—also known as anaphylaxis—after getting a COVID-19 vaccine. As an example, an allergic reaction is considered severe when a person needs to be treated with epinephrine or EpiPen© or if they must go to the hospital.
To protect yourself, follow these recommendations:
· Wear a mask over your nose and mouth.
· Stay at least 6 feet away from others.
· Avoid crowds.
· Avoid poorly ventilated spaces.
· Wash your hands often.
Get more information about these and other steps you can take to protect yourself and others from COVID-19.
Yes. Due to the severe health risks associated with COVID-19 and the fact that reinfection with COVID-19 is possible, you should be vaccinated regardless of whether you already had COVID-19 infection. If you were treated for COVID-19 symptoms with monoclonal antibodies or convalescent plasma, you should wait 90 days before getting a COVID-19 vaccine. Talk to your doctor if you are unsure what treatments you received or if you have more questions about getting a COVID-19 vaccine.
· Experts do not yet know how long someone is protected from getting sick again after recovering from COVID-19. The immunity someone gains from having an infection, called “natural immunity,” varies from person to person. It is rare for someone who has had COVID-19 to get infected again. It also is uncommon for people who do get COVID-19 again to get it within 90 days of when they recovered from their first infection. We won’t know how long immunity produced by vaccination lasts until we have more data on how well the vaccines work.
· Both natural immunity and vaccine-induced immunity are important aspects of COVID-19 that experts are working to learn more about, and CDC will keep the public informed as new evidence becomes available.
People who are pregnant and part of a group recommended to receive the COVID-19 vaccine may choose to be vaccinated. If you have questions about getting vaccinated, talking with a healthcare provider may might help you make an informed decision. While breastfeeding is an important consideration, it is rarely a safety concern with vaccines.
· No data are available yet on the safety of COVID-19 vaccines in lactating women or on the effects of mRNA vaccines on breastfed infants or on milk production/excretion. mRNA vaccines are not thought to be a risk to breastfeeding infants. People who are breastfeeding and are part of a group recommended to receive a COVID-19 vaccine, such as healthcare personnel, may choose to be vaccinated.
· To make sure that more information is gathered regarding the safety of these vaccines when administered during pregnancy, pregnant people are encouraged to enroll in v-safe, CDC’s new smartphone-based tool being used to check-in on people’s health after they receive a COVID-19 vaccine. If pregnant people report health events through v-safe after vaccination, someone from CDC may call to check on them and get more information. Additionally, pregnant people enrolled in v-safe will be contacted by CDC and asked to participate in a pregnancy registry that will monitor them through pregnancy and the first 3 months of infancy. Learn more about COVID-19 vaccination considerations for people who are pregnant or breastfeeding
People with underlying medical conditions can receive the FDA-authorized COVID-19 vaccines provided they have not had an immediate or severe allergic reaction to a COVID-19 vaccine or to any of the ingredients in the vaccine. ·
Learn more about vaccination considerations for persons with underlying medical conditions. Vaccination is an important consideration for adults of any age with certain underlying medical conditions because they are at increased risk for severe illness from the virus that causes COVID-19.
If you get a COVID-19 vaccine and you think you might be having a severe allergic reaction after leaving the vaccination site, seek immediate medical care by calling 911.
You can report side effects and reactions using either v-safe or the Vaccine Adverse Event Reporting System (VAERS.)
· V-safe is a new smartphone-based, after-vaccination health checker for people who receive COVID-19 vaccines. V-safe uses text messaging and web surveys from CDC to check in with vaccine recipients following COVID-19 vaccination. V-safe also provides second vaccine dose reminders if needed, and telephone follow up to anyone who reports medically significant (important) adverse events.
· Vaccine Adverse Event Reporting System (VAERS)external icon is the national system that collects reports from healthcare professionals, vaccine manufacturers, and the public of adverse events that happen after vaccination; reports of adverse events that are unexpected, appear to happen more often than expected, or have unusual patterns are followed up with specific studies. Reports to VAERS help CDC monitor the safety of vaccines. If experts detect an unexpected adverse event, they quickly study it further to assess whether it is a true safety concern. Experts then decide whether changes are needed in U.S. vaccine recommendations. This monitoring is critical to help ensure that the benefits continue to outweigh the risks for people who receive vaccines.
As soon as the first vaccine was approved and administered, internet scams taking advantage of the moment started to surface. Unfortunately, there have been reports of fraudulent scams due to the demand of the COVID vaccine, The FBI recently issued a public warning to be on the lookout for such schemes, including ones offering access to early vaccination in exchange for a fee, requests to put your name on a vaccine waiting list, and vaccine ads via social media, email, phone calls, or other sketchy sources.
· Best practice is to check your state’s health department website for up-to-date info on authorized vaccine distribution channels and then only obtain a vaccine through those channels.
· You can also always check the FDA and CDC websites or contact your doctor directly.
Testing is available for any community member age 5 and over.
The testing site will operate Monday – Saturday from 9:30 AM to 4:00 PM
The site is located at the UW Sports Factory Upper Parking Lot at 305 S Madison St. Rockford IL
For more information, call OSH at (844) 871‑5651.

 This outbreak has had far-reaching effects, including the public at large as well as on travel, supply chains, and economies locally as well as globally.
This outbreak has had far-reaching effects, including the public at large as well as on travel, supply chains, and economies locally as well as globally.
Many people sheltering at home today in our community naturally have questions: Am I safe? Are my kids safe? Will my savings last, if I have any? When will my children get back to school? When am I realistically going to be able to get back to work? While the short-term future is yet unknown, the leadership Team of the Rockford Housing Authority has taken many steps to provide safely for our RHA residents and our service providers.
As you are aware all RHA offices are closed to the public, and until further notice, all public meetings and personal contact interactions are canceled. This includes all internal and external meetings, events, briefings, HQS inspections that are not health and safety-related, work-order services that are not health and safety-related, and resident activities. The Rockford Housing Authority will continue to remain vigilant about the possible spread of this virus through person to person contact.
Illinois Governor JB Pritzker provided an update on taking a public health approach to safely reopen our state on a region-by-region basis. There are four regions such as northeast Illinois, north-central Illinois, central Illinois, and southern Illinois. The northern Illinois region, including Winnebago, Boone, Ogle, Stephenson, and Lee counties, are in the North-Central region.
Governor JB Pritzker announced a 5-phase plan to re-open Illinois. We are currently in the Phase 2-Flattening phase.
The governor has announced that phase 3-recovery will include reopening businesses such as manufacturing, offices, hair salons, barbershops, and retail stores. To enter phase 3 the rate of infection among those tested, the number of patients admitted to the hospital, and the number of patients needing ICU beds must be stable or declining. Gatherings of 10 people or less with face coverings and social distancing are still required. As of now, there are no dates for Phases 4 or 5, but the earliest a region can get to Phase 3 is May 29th.
For the entire special report on the Coronavirus Briefing from Gov. J.B. Pritzker, Wednesday, May 6, 2020, please follow this link: https://news.wttw.com/chicago-tonight-live-stream-special-report
Click the following to download the complete Restore Illinois PDF: Restore Illinois – A Public Health Approach To Safely Reopen Our State 050620
Illinois officials say a state helpline has been set up to provide emotional support and quick answers to questions about the coronavirus pandemic. Illinoisans can text “TALK” to 55-2020 (or “HABLAR” for Spanish), and within 24 hours, they will receive a call from a counselor. Residents can also text keywords such aS “UNEMPLOYMENT,” “FOOD,” or “SHELTER,” to the same number to receive additional information about those topics
“Illinois has had a mask mandate since May 1 of this year, and in most establishments, people are adhering to it, but it’s important that we treat hospitality employees just as you would in any retail store or establishment,” Pritzker said. “This new requirement asks a little bit more of our residents dining out in order to protect their health and safety and that of our frontline hospitality workers.”
Beginning August 26, 2020, patrons must wear a face-covering during all interactions with staff at Illinois bars, restaurants and other food service areas under new statewide rules announced Monday. The updated regulations make the commonsense courtesy mandatory for customers for the first time.
Illinois Department of Public Health Director Dr. Ngozi Ezike said the updated guidelines aim to make it clear that face coverings should be worn any time people interact with someone outside of their immediate circle. She said going out for food or drinks should not serve as an excuse for people not to take precautions against COVID-19.
“Stop wearing your face coverings incorrectly. You’re literally contributing to infection transmission by doing so, and by contributing to infection transmission, potentially to an additional life that will be lost,” Ezike said. Your mask must cover your entire nose and mouth at all times. If it slips down your mask may be too small.
“To the people who say that face coverings don’t work: You are simply wrong,” she added. “It doesn’t matter what video you saw on the internet or the fake headline you read, please know that face coverings do save lives, but they must be used in conjunction with social distancing and hand-washing.”
The governor said the policy was aimed at reducing the risk of airborne transmission by restricting the amount of droplets in the air.
“Remember how COVID-19 transmits. It is essentially your saliva becoming aerosolized when you’re speaking,” Pritzker said. “The idea is to make sure that the masks are being worn when the servers are coming to your table so you’re not exposing them, making sure that at all times when you’re not eating that you’re wearing a mask, trying to, again, keep the aerosolization and, more importantly, the viral load down.”
Under existing rules implemented as part of Phase 4 of Pritzker’s Restore Illinois re-opening plan, all patrons are required to wear masks when on the premises of bars or restaurants except while eating or drinking at a table or bar. The updated guidelines are intended to make interactions with patrons and staff safer, according to state officials, who said it was crafted along with trade groups like the Illinois Restaurant Association, or IRA.
Due to recent outbreaks within our community and in Region 1, we need to revert back to all exempt staff working 100% remote. This will include all staff, community, and public meetings being held virtually. During this crisis, all management team members will work remotely from their homes. Frontline property management staff will work a 50/50 schedule, to ensure that our development offices are staffed. Our maintenance team will focus on vacant unit turns, outdoor work, and respond to emergency maintenance concerns.
However, we will ensure that the entire RHA Team remains accessible to meet the needs of our residents, contractors, and the community.
We will continue to update you, and we encourage you to use all available resources to stay well. The measures we take now will help us to serve you, our residents, and the Rockford community.
For Administrative needs, you may phone 815-489-8500.
During this unprecedented time, the Rockford Housing Authority executive team has taken proactive steps to ensure our employees, clients, and community’s safety. To keep our RHA staff safe, the RHA Leadership Team has instituted numerous protocols that are in place that align with all government regulations aimed at limiting the spread of disease and sickness.
We have educated our employees on Covid19 and the best practices for preventing infection, including frequent hand washing accompanied by social distancing. RHA has ongoing sanitized services at all RHA locations regularly. We have provided access to soap, masks, and available hand- sanitizers at all times for our residents and RHA staff.
During these uncertain times, the RHA Leadership will continue to be diligent in our residents’ services and care for their wellbeing. These are undoubtedly uncharted waters for us all. Our continued hope is for you to remain healthy and safe. Your support through these difficult times is heartfelt. Please stay safe, stay healthy as we all move forward to normalcy.
THANK YOU!
THE RHA LEADERSHIP TEAM
Illinois residents should work from home whenever possible and participate only in “essential” activities over the next three weeks — including the Thanksgiving holiday period — as coronavirus trends continue in the wrong direction.
The Illinois Department of Public Health made several recommendations Wednesday for residents to “stay at home as much as possible” over the next three weeks, but officials stopped short of issuing any orders to that effect.
The IDPH urged employers to allow their workers to stay home and for people to only leave their homes for “necessary and essential activities,” including work that cannot be done remotely, as well getting groceries, coronavirus tests or other necessities.
Officials are also imploring residents to limit their travels for the next three weeks, including over the Thanksgiving holiday period, which could “present a high risk of spreading the infection,” the IDPH said in a release.
“Our goal is to reduce transmission as we head into the holidays so businesses and schools can remain open,” IDPH officials said.
As with all other agencies throughout our country, we are doing our best to navigate the uncharted territory of COVID-19. Your executive team continues to monitor this crisis and adjust our policies and practices where needed. Amid today’s challenges, our employee’s safety, health, and the well-being of our residents remain a top priority. As this situation evolves, we will continue to update you, and we encourage you to use all available resources to stay well educated on practical measures you can take to limit your exposure to this virus.
The majority of the population that we serve is one that is the most vulnerable to this virus. Therefore, we must remain in operation and be vigilant in our practices to maintain a safe and sanitary environment. We will continue to follow the methods that were put in place recently until further notice.

Yes, our sites and main office are staffed. However, following Federal, State, and local declarations and the Center for Disease Control’s recommendations, offices are currently closed for in-person visits.
We ask that residents contact their Property Manager, Specialist or Caseworker via phone or email.
If an appointment is needed one will be scheduled.
NOTE— General Line: 815-489-8500
Yes, rent is due the 1st of each month and should be paid by the 5th in order to avoid late fees or future legal action.
Be sure to contact your Property Manager, Specialist or Caseworker. Provide documentation and/or information regarding the change in income per RHA staff instructions. Staff will then take the necessary actions to complete the rent adjustment.
Currently all inspections outside of initials and health/safety are currently on hold.
RHA will mail you an inspection appointment letter once inspections resume. Our pest control contractor has stated that they will continue to treat units as scheduled. As always, please report any issues to your property management office as soon as possible.
Yes, please continue to report any/all issues to your property management office. “Emergency and Health & Safety” issues are our priority.
NOTE: During normal working hours (M-F 8AM-5PM) contact management office. After hour issues, be sure to call 815-489-8585.
It’s your hands, anytime you enter your home from outside, after using the bathroom, and after sneezing, coughing, or blowing your nose, wash with soap and water for at least 20 seconds. Your next priority should be your phone. “At my house, we clean phones first because after you wash your hands you don’t want to be grabbing a dirty phone. Most phones can withstand a quick swipe with isopropyl alcohol or some kind of rubbing alcohol — the 70% alcohol you can get at the drugstore.”
—Paul Pottinger, MD, an infectious disease specialist in the department of medicine at the University of Washington in Seattle.
Wear disposable gloves to clean and disinfect. Clean the area or item with soap and water or another detergent if it is dirty. Then, use a household disinfectant. The virus dies with the application of one of many products approved by the EPA and good old-fashioned elbow grease to make sure that product gets into every little crack.
Here are links for information of the List N: Disinfectants for Use Against SARS-CoV-2 Other COVID-19 Resources
This list includes products that meet EPA’s criteria for use against SARS-CoV-2, the novel coronavirus that causes the disease COVID-19.
The coronavirus outbreak is rapidly evolving. To stay informed, check the U.S. Centers for Disease Control and Prevention as well as our local health department for updates. Please see the many additional resources below.
The enemy we are facing is very good at what it does; we are not failing. We need everyone to hold the line as the epidemic inevitably gets worse with social distancing. The Centers for Disease Control and Prevention (CDC) officials are suggesting to limit a person’s risk of exposure or of spreading the virus, which the CDC states that it is transmitted through droplets from coughs and sneezes between people who are up to six feet apart from one another —This is “social distancing.”
The Links below are compiled resources on how to prevent spreading the disease, help for vulnerable populations, and the most current information you may find useful.

 CDC, “Interim Guidance for Homeless Shelters”
CDC, “Interim Guidance for Homeless Shelters”Web guide researching drugs, alcohol, addiction, and recovery

“If an individual is experiencing symptoms of COVID-19 including fever, shortness of breath and cough, they call their healthcare provider.
The healthcare provider will consider these symptoms, travel history, possible exposure to a known case, and any underlying health conditions specific to that patient when evaluating the need for testing for COVID-19. If COVID-19 testing is needed, healthcare providers collect the specimens that are then sent to a State or private lab for testing.
The healthcare provider will determine if you need to be tested for COVID0-19 and may recommend that you stay home and provide self-care if you have mild symptoms. Those individuals who have no symptoms, do not need to be tested.
The positive cases of COVID-19 reported by the Illinois Department of Public Health and the Winnebago County Health Department include all positive tests that were submitted to the state or private lab for testing.”

Both this disease and the vaccine are new. We do not know how long protection lasts for those who get infected or those who are vaccinated. Experts are working to learn more about both natural immunity and vaccine-induced immunity. CDC will keep the public informed as new evidence becomes available.
· The potential serious risk COVID-19 infection poses to them and their loved ones if they get the illness or spread it to others. Remind them of the potential for long-term health issues after recovery from COVID-19 disease.
· Scientists are still learning more about the virus that causes COVID-19. And it is not known whether getting COVID-19 disease will protect everyone against getting it again, or, if it does, how long that protection might last.
· The vaccine was tested in large clinical trials and what is currently known about its safety and effectiveness.
· The vaccine is not a perfect fix. You will still need to practice other precautions like wearing a mask, social distancing, handwashing, and other hygiene measures until public health officials say otherwise.
COVID-19 vaccines were tested in large clinical trials to make sure they meet safety standards. Many people were recruited to participate in these trials to see how the vaccines offers protection to people of different ages, races, and ethnicities, as well as those with different medical conditions.
· The Food and Drug Administration (FDA) carefully reviews all safety data from clinical trials and an authorizes emergency vaccine use only when the expected benefits outweigh potential risks.
· The Advisory Committee on Immunization Practices (ACIP) reviews all safety data before recommending any COVID-19 vaccine for use.
· FDA and CDC will continue to monitor the safety of COVID-19 vaccines, to make sure even very rare side effects are identified.
According to the CDC, the COVID-19 vaccine will be given to U.S. citizens at no cost, Yacoub confirms. Some vaccine providers may decide to charge an additional fee for administering the shot, but this fee can be reimbursed by recipients’ insurance, or, if uninsured, the Health Resources and Services Administration’s Provider Relief Fund
Most people do not have serious problems after being vaccinated. We will understand more about mild side effects of the COVID-19 vaccine before we start to use it. However, your arm may be sore, red, or warm to the touch. These symptoms usually go away on their own within a week. Some people report getting a headache or fever when getting a vaccine. These side effects are a sign that your immune system is doing exactly what it is supposed to do. It is working and building up protection to disease.
· A fever is a potential side effect and when they should seek medical care.
· Symptoms typically go away on their own within a week. Also let them know when they should seek medical care if their symptoms don’t go away.
· The vaccine cannot give someone COVID-19.
· The side effects are a sign that the immune system is working.
COVID-19 vaccines are being tested in large clinical trials to assess their safety. However, it does take time, and more people getting vaccinated before we learn about very rare or long-term side effects. That is why safety monitoring will continue. CDC has an independent group of experts that reviews all the safety data as it comes in and provides regular safety updates. If a safety issue is detected, immediate action will take place to determine if the issue is related to the COVID-19 vaccine and determine the best course of action.
· The FDA and CDC are continuing to monitor safety, to make sure even long-term side effects are identified.
· COVID-19 vaccines will be continuously monitored for safety after authorization, and ACIP will take action to address any safety problems detected.
All but one of the COVID-19 vaccines currently in phase 3 clinical trials use two shots. The same vaccine brand must be used for both shots.
· Nearly all COVID-19 vaccines being studied in the United States require two shots. The first shot starts building protection, but everyone has to come back a few weeks later for the second one to get the most protection the vaccine can offer.
· Two shots are generally needed to provide the best protection against COVID-19 and that the shots are given several weeks apart. The first shot primes the immune system, helping it recognize the virus, and the second shot strengthens the immune response.
The two COVID-19 vaccines currently available in the United States do not contain eggs, preservatives, or latex.
For a full list of ingredients, please see each vaccine’s,
Fact Sheet for Recipients & Caregivers:
· Pfizer-BioNTech COVID-19 vaccineexternal
· Moderna COVID-19 vaccineexternal
Notable Differences:
· Age minimum: The vaccine developed by Pfizer and BioNTech is approved for people age 16 and older, and the vaccine developed by Moderna is approved for people age 18 and older
· Storage requirements: Moderna does not require ultra-cold storage [like Pfizer doses do], making it easier to store while the Moderna vaccine can be stored in a freezer or refrigerator, the Pfizer vaccine needs to be stored in a special container in very cold temperatures. This discrepancy won’t affect you directly but is more the concern of healthcare facilities.
Serious problems from vaccination can happen, but they are rare. CDC has learned of reports that some people have experienced severe allergic reactions—also known as anaphylaxis—after getting a COVID-19 vaccine. As an example, an allergic reaction is considered severe when a person needs to be treated with epinephrine or EpiPen© or if they must go to the hospital.
To protect yourself, follow these recommendations:
· Wear a mask over your nose and mouth.
· Stay at least 6 feet away from others.
· Avoid crowds.
· Avoid poorly ventilated spaces.
· Wash your hands often.
Get more information about these and other steps you can take to protect yourself and others from COVID-19.
Yes. Due to the severe health risks associated with COVID-19 and the fact that reinfection with COVID-19 is possible, you should be vaccinated regardless of whether you already had COVID-19 infection. If you were treated for COVID-19 symptoms with monoclonal antibodies or convalescent plasma, you should wait 90 days before getting a COVID-19 vaccine. Talk to your doctor if you are unsure what treatments you received or if you have more questions about getting a COVID-19 vaccine.
· Experts do not yet know how long someone is protected from getting sick again after recovering from COVID-19. The immunity someone gains from having an infection, called “natural immunity,” varies from person to person. It is rare for someone who has had COVID-19 to get infected again. It also is uncommon for people who do get COVID-19 again to get it within 90 days of when they recovered from their first infection. We won’t know how long immunity produced by vaccination lasts until we have more data on how well the vaccines work.
· Both natural immunity and vaccine-induced immunity are important aspects of COVID-19 that experts are working to learn more about, and CDC will keep the public informed as new evidence becomes available.
People who are pregnant and part of a group recommended to receive the COVID-19 vaccine may choose to be vaccinated. If you have questions about getting vaccinated, talking with a healthcare provider may might help you make an informed decision. While breastfeeding is an important consideration, it is rarely a safety concern with vaccines.
· No data are available yet on the safety of COVID-19 vaccines in lactating women or on the effects of mRNA vaccines on breastfed infants or on milk production/excretion. mRNA vaccines are not thought to be a risk to breastfeeding infants. People who are breastfeeding and are part of a group recommended to receive a COVID-19 vaccine, such as healthcare personnel, may choose to be vaccinated.
· To make sure that more information is gathered regarding the safety of these vaccines when administered during pregnancy, pregnant people are encouraged to enroll in v-safe, CDC’s new smartphone-based tool being used to check-in on people’s health after they receive a COVID-19 vaccine. If pregnant people report health events through v-safe after vaccination, someone from CDC may call to check on them and get more information. Additionally, pregnant people enrolled in v-safe will be contacted by CDC and asked to participate in a pregnancy registry that will monitor them through pregnancy and the first 3 months of infancy. Learn more about COVID-19 vaccination considerations for people who are pregnant or breastfeeding
People with underlying medical conditions can receive the FDA-authorized COVID-19 vaccines provided they have not had an immediate or severe allergic reaction to a COVID-19 vaccine or to any of the ingredients in the vaccine. ·
Learn more about vaccination considerations for persons with underlying medical conditions. Vaccination is an important consideration for adults of any age with certain underlying medical conditions because they are at increased risk for severe illness from the virus that causes COVID-19.
If you get a COVID-19 vaccine and you think you might be having a severe allergic reaction after leaving the vaccination site, seek immediate medical care by calling 911.
You can report side effects and reactions using either v-safe or the Vaccine Adverse Event Reporting System (VAERS.)
· V-safe is a new smartphone-based, after-vaccination health checker for people who receive COVID-19 vaccines. V-safe uses text messaging and web surveys from CDC to check in with vaccine recipients following COVID-19 vaccination. V-safe also provides second vaccine dose reminders if needed, and telephone follow up to anyone who reports medically significant (important) adverse events.
· Vaccine Adverse Event Reporting System (VAERS)external icon is the national system that collects reports from healthcare professionals, vaccine manufacturers, and the public of adverse events that happen after vaccination; reports of adverse events that are unexpected, appear to happen more often than expected, or have unusual patterns are followed up with specific studies. Reports to VAERS help CDC monitor the safety of vaccines. If experts detect an unexpected adverse event, they quickly study it further to assess whether it is a true safety concern. Experts then decide whether changes are needed in U.S. vaccine recommendations. This monitoring is critical to help ensure that the benefits continue to outweigh the risks for people who receive vaccines.
As soon as the first vaccine was approved and administered, internet scams taking advantage of the moment started to surface. Unfortunately, there have been reports of fraudulent scams due to the demand of the COVID vaccine, The FBI recently issued a public warning to be on the lookout for such schemes, including ones offering access to early vaccination in exchange for a fee, requests to put your name on a vaccine waiting list, and vaccine ads via social media, email, phone calls, or other sketchy sources.
· Best practice is to check your state’s health department website for up-to-date info on authorized vaccine distribution channels and then only obtain a vaccine through those channels.
· You can also always check the FDA and CDC websites or contact your doctor directly.

In the newly released stimulus package, there’s an initial 350 billion dollars for small business relief. This program waives many of the traditional SBA requirements, and it’s available for sole proprietors up to businesses with 500 employees.
Under the bill, you can use funds from the loans to pay your employees and cover certain other expenses like utilities or insurance premiums. And you can apply for loan forgiveness if you meet certain requirements. Additionally, businesses applying for these loans can receive an advance of $10,000 within three days of submitting their application.
Contact your local financial institution or find an approved lender using Lender Match.
The SBA Coronavirus Center has more information on requirements, processes, and options.
They are also offering some creative solutions for schools and nonprofits. You can learn more about their platform and learn how to use it in their coronavirus support center.
For Administrative needs, you may phone 815-489-8500.
You can also reach out via the RHA WEBSITE.
For any questions or concerns regarding the above practices, please call your program manager or Director.
In case of criminal or life-threatening emergency Please Dial 911
If you have any information or concerns to share with
security please call:
Confidential Hotline: 815-489-8549
Rockford Non-Emergency: 815-966-2900
As with all other agencies throughout our country, we are doing our best to navigate the uncharted territory of CoVid19. Your executive team continues to monitor this crisis and adjust our policies and practices where needed. Amid today’s challenges, our employee’s safety, health, and the well-being of our residents remain a top priority. As this situation evolves, we will continue to update you, and we encourage you to use all available resources to stay well educated on practical measures you can take to limit your exposure to this virus.
The majority of the population that we serve is one that is the most vulnerable to this virus. Therefore, we must remain in operation and be vigilant in our practices to maintain a safe and sanitary environment. We will continue to follow the methods that were put in place recently until further notice.

As you are fully aware, when someone who is infected coughs or sneezes, they send droplets containing the virus into the air, and a healthy person can then breathe in those droplets. However, as you may know, you can also catch the virus if you touch a surface or object that has the virus on it and then touch your mouth, nose, or eyes. This could be a contaminated roll of toilet paper, a doorknob, or even a plastic water bottle. Find out more here and find a downloadable 11×17 poster to hang up in your house, office, or place of business.
The Links below are compiled resources on how to prevent spreading the disease, help for vulnerable populations, and the most current information you may find useful.

 CDC, “Interim Guidance for Homeless Shelters”
CDC, “Interim Guidance for Homeless Shelters”Illinois Department of Public Health
Click HERE to view grocery store hours. Note the special times set aside for senior citizens and at-risk people to shop.
Click HERE for a list of restaurants that remain open for delivery and/or carry out. This list will be updated continuously.
Click HERE for information from RPS205 regarding distribution of student meals.
The RPS 205 Nutrition Services team will provide meals to students on Mondays and Thursdays from 9-10:15 a.m. starting Monday, April 6.
On Mondays, families will receive breakfast and lunch for 3 days: Monday, Tuesday and Wednesday. On Thursdays, families will receive breakfast and lunch for 3 days: Thursday, Friday and Saturday. All children ages 2-18 can receive these prepackaged meals.
Meals will be available at eight locations:
Click HERE for information regarding United Way’s 211 program that connects people to resources. (Additionally, United Way of Rock River Valley has established a COVID-19 Emerging Needs Fund to support the needs of residents and their children to help alleviate hardships they may be experiencing due to the COVID -19 pandemic. An anonymous donor helped establish the fund with an initial $10,000 gift. Contributions, large and small, are being sought from area businesses and individuals.
There are local agencies offering childcare support and services during the COVID-19 crisis. They are listed below, along with the specifics on their availability.

The Northern Illinois Food Bank is offering support, including a list of the food pantries and programs nearest you. Go to solvehungertoday.org/coronavirus for more.
I need additional help. Who do I contact?
If you’re in need of assistance due to hardships presented by the COVID-19 pandemic, you can call 211 any time of day to be put in touch with local resources and assistance.
Click HERE for a list of “Museums, Zoos, and Theme Parks Offering Virtual Tours.”

A properly fitted mask can provide some added protection over a poorly fitting mask for both the wearer and other people. The primary intent of mask use is to suppress the spread of virus from the wearer to other people. Because COVID-19 can be spread by people who display characteristic symptoms and by those who do not exhibit any symptoms, broad mask use is encouraged to minimize the spread from those who are sick (or potentially sick) to others.
The mask, if worn properly and consistently, also helps protect healthy people from catching the disease when they are in close proximity to people who are sick. It may also provide protection to the wearer from aerosols that persist in poorly ventilated environments, such as an elevator.
Information about how long virus-carrying droplets can persist in the air is being updated regularly. Some research suggests that droplets can remain airborne for multiple hours. So do your part to protect yourself and others by wearing well-fitting, protective masks.
The simple answer is NO. Wearing a mask, in part, is meant to protect your respiratory system (your lungs, throat, and sinuses) from direct exposure to airborne droplets and particles that may contain the virus.
To do this, one must protect the primary entry points to your lungs and throat—your nose and mouth. Therefore, leaving your nose exposed will provide an easy pathway for airborne particles to enter your system (by inhaling through your nose) or for droplets to exit your system (by exhaling, sneezing, etc.), potentially endangering those around you.
Absolutely. Even with a mask, you should still make every effort to stay at least 6 feet away from people who don’t live with you. Masking is only one layer of protection, and it’s an imperfect one. Social distancing isn’t foolproof, either, but the more layers of protection you can employ, the safer you’ll make yourself and everyone else around you.
 This outbreak has had far-reaching effects, including the public at large as well as on travel, supply chains, and economies locally as well as globally.
This outbreak has had far-reaching effects, including the public at large as well as on travel, supply chains, and economies locally as well as globally.
Some people in your family may need to take more steps to be better protected from COVID-19, including
Illinois officials say a state helpline has been set up to provide emotional support and quick answers to questions about the coronavirus pandemic. Illinoisans can text “TALK” to 55-2020 (or “HABLAR” for Spanish), and within 24 hours, they will receive a call from a counselor. Residents can also text keywords such aS “UNEMPLOYMENT,” “FOOD,” or “SHELTER,” to the same number to receive additional information about those topics
 are safe and effective.
are safe and effective.Three COVID-19 vaccines are authorized or approved for use in the United States to prevent COVID-19. Pfizer-BioNTech or Moderna (COVID-19 mRNA vaccines) are preferred. You may get Johnson & Johnson’s Janssen COVID-19 vaccine in some situations.
COVID-19 by County: COVID-19 Community Levels are a new tool to help you and communities decide what prevention steps to take based on hospitalizations and cases.
Check your community level.
Strategies to reduce the spread of COVID-19 and maintain safe operations in schools, child care programs, and institutions of higher education.
Yes, our sites and main office are staffed. However, masks are stil required in RHA deveopments and offices
We ask that residents contact their Property Manager, Specialist or Caseworker via phone or email.
If an appointment is needed one will be scheduled.
NOTE— General Line: 815-489-8500
Yes, rent is due the 1st of each month and should be paid by the 5th in order to avoid late fees or future legal action.
Be sure to contact your Property Manager, Specialist or Caseworker. Provide documentation and/or information regarding the change in income per RHA staff instructions. Staff will then take the necessary actions to complete the rent adjustment.
Currently all inspections outside of initials and health/safety are currently on hold.
RHA will mail you an inspection appointment letter once inspections resume. Our pest control contractor has stated that they will continue to treat units as scheduled. As always, please report any issues to your property management office as soon as possible.
Yes, please continue to report any/all issues to your property management office. “Emergency and Health & Safety” issues are our priority.
NOTE: During normal working hours (M-F 8AM-5PM) contact management office. After hour issues, be sure to call 815-489-8585.
It’s your hands, anytime you enter your home from outside, after using the bathroom, and after sneezing, coughing, or blowing your nose, wash with soap and water for at least 20 seconds. Your next priority should be your phone. “At my house, we clean phones first because after you wash your hands you don’t want to be grabbing a dirty phone. Most phones can withstand a quick swipe with isopropyl alcohol or some kind of rubbing alcohol — the 70% alcohol you can get at the drugstore.”
—Paul Pottinger, MD, an infectious disease specialist in the department of medicine at the University of Washington in Seattle.
Wear disposable gloves to clean and disinfect. Clean the area or item with soap and water or another detergent if it is dirty. Then, use a household disinfectant. The virus dies with the application of one of many products approved by the EPA and good old-fashioned elbow grease to make sure that product gets into every little crack.
Here are links for information of the List N: Disinfectants for Use Against SARS-CoV-2 Other COVID-19 Resources
This list includes products that meet EPA’s criteria for use against SARS-CoV-2, the novel coronavirus that causes the disease COVID-19.
The coronavirus outbreak is rapidly evolving. To stay informed, check the U.S. Centers for Disease Control and Prevention as well as our local health department for updates. Please see the many additional resources below.
The enemy we are facing is very good at what it does; we are not failing. We need everyone to hold the line as the epidemic inevitably gets worse with social distancing. The Centers for Disease Control and Prevention (CDC) officials are suggesting to limit a person’s risk of exposure or of spreading the virus, which the CDC states that it is transmitted through droplets from coughs and sneezes between people who are up to six feet apart from one another —This is “social distancing.”

To continue to create strategic partnerships with community stakeholders, design a diverse housing portfolio, leverage social service programming to unite and ensure residents are provided with safe and nurturing environments that lead to self-sufficiency, responsibility, and individual empowerment.
The RHA April InFocus Newsletter is Now Out!
View articles about Fair Housing Month 2024, Laura Snyder, RHA CEO's Message, and a recap of the Women of Influence event! View the rest of the RHA Newsletter here: https://rockfordha.org/newsletters/
#RHA #MovingForwardTogether
Diversity Month is more than just a monthly recognition- it's about recognizing the inherent value of each individual and the contributions they bring to our community. This Diversity Month, let's commit to promoting equity, diversity, and inclusion in all aspects of our lives.
Happy Administrative Professionals' Day to Angel Mackey and Jennifer Matlick! 🌟
Thank you for all that you do to keep RHA running smoothly!
View the full RHA Administrative Professional's Day Appreciation Blog here: https://rockfordha.org/administrative-professionals-day/

Within 5 years the RHA will re-establish itself as high performing agency that is a leader in housing and sustainable communities by developing additional, non-HUD revenue streams, increasing our asset base and offering state of the art resident initiatives.